 
The first phase is the feasibility phase of the study where one eye will be treated using non-FDA approved investigational SILK procedure and the other eye will be treated with FDA-approved laser vision correction surgery. 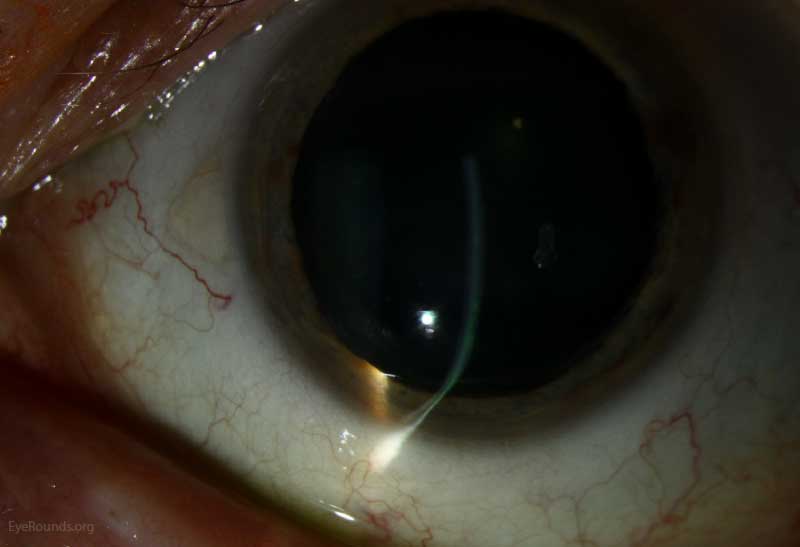
This will be a prospective, multicenter, research study in which up to 90 consecutive patients scheduled to undergo small incision lenticule keratomileusis (SILK) at Stanford and 200 patients study-wide for the correction of myopia (nearsightedness) with and without astigmatism will be enrolled. Two hundred patients will be enrolled study wide at up to 15 study sites in the United States and part of the multicenter clinical trial. You will be one of up to 90 near-sighted patients at Stanford to undergo treatment in this clinical research trial. You will have one eye or both eyes treated with small incision lenticule keratomileusis using the Elita femtosecond laser system. SILK surgery has been performed in 154 patients outside of the United States. It has been used in humans outside the United States. The Elita femtosecond laser used to perform SILK surgery is not FDA-approved. The excimer laser system precisely ablates (removes) corneal tissue to reduce or eliminate your nearsightedness, farsightedness, astigmatism and mixed astigmatism. The femtosecond laser is used to create the corneal flap during the first step of the LASIK procedure. The cornea is the clear front portion of the eye. Small incision lenticule keratomileusis is a one-step procedure consisting of initial creation of a corneal flap (a thin slice of the cornea) and subsequent corneal ablation (removal of tissue) with an excimer laser (a non-thermal laser). All rights reserved.You are invited to participate in a research study evaluating the safety and effectiveness of the Johnson and Johnson femtosecond laser system used to perform small incisions lenticule keratomileusis nearsightedness with and without astigmatism (a non-spherical shape) as part of a multicenter FDA clinical trial. This review describes the clinical features of PMD, its differential diagnosis and various management strategies presently available.Ĭopyright © 2010 British Contact Lens Association. Since patients with PMD make poor candidates for laser vision correction, an awareness of the topographical and slit-lamp features of PMD will be useful to clinicians screening for signs of corneal abnormality before corneal refractive surgery. Several surgical procedures have been used in an attempt to improve visual acuity when spectacles and contact lenses do not provide adequate vision correction. The vast majority of PMD patients are managed using spectacles and contact lenses. 
In rare cases, patients may present with a sudden loss of vision and excruciating ocular pain due to corneal hydrops or spontaneous perforation. Visual signs and symptoms include longstanding reduced visual acuity or increasing against-the-rule irregular astigmatism leading to a slow reduction in visual acuity. Unless corneal topography is evaluated, early forms of PMD may often be undetected however, in the later stages PMD can often be misdiagnosed as keratoconus. Ocular signs and symptoms of patients with PMD differ depending on the severity of the condition. The prevalence and aetiology of this disorder remain unknown. The condition is most commonly found in males and usually appears between the 2nd and 5th decades of life affecting all ethnicities. Pellucid marginal corneal degeneration (PMD) is a rare ectatic disorder which typically affects the inferior peripheral cornea in a crescentic fashion. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
